 This is another recent review from Am Fam Physician:
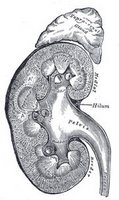
This is another recent review from Am Fam Physician:Chronic kidney disease (CKD) affects 27 million adults in the U.S. It increases risk of cardiovascular disease and stroke.
Patients should be assessed annually to determine whether they are at increased risk of developing chronic kidney disease (CKD).
Risk factors for CKD include:
- diabetes mellitus
- hypertension
- older age
- cardiovascular disease
- family history of chronic kidney disease
- ethnic and racial minority status
Tests for CKD:
- Serum creatinine levels can be used to estimate the glomerular filtration rate (GFR)
- Spot urine testing can detect proteinuria
Staging of CKD is based on estimated glomerular filtration rate (GFR). Evaluation should focus on the specific type of CKD and identifying complications related to the disease stage.
When to refer to a nephrologist?
The patients with the following characteristics should be referred to a nephrologist:
- estimated glomerular filtration rates less than 30 mL per minute per 1.73 m2
- significant proteinuria
- rapid loss of kidney function
References:
Chronic Kidney Disease: Detection and Evaluation. Baumgarten M, Gehr T. Am Fam Physician. 2011 Nov 15;84(10):1138-1148.
Nephrology Cases